What to Expect From an Epidural Steroid Injection
A plain-language walkthrough of the procedure — what happens before, during, and after, and what most patients experience in the days that follow.
What an epidural steroid injection actually delivers
An epidural steroid injection (ESI) places a corticosteroid — an anti-inflammatory medication — directly into the epidural space of the spine. The epidural space is the outermost layer of the spinal canal, sitting just outside the protective membrane (the dura) that surrounds the spinal cord and nerve roots.
The target is inflammation. When a disc herniates or degenerates, or when the spinal canal narrows, nerve roots can become compressed and inflamed. Inflamed nerve tissue signals pain. Delivering corticosteroid directly to that site suppresses the local inflammatory response, which is why the procedure can produce pain relief that oral anti-inflammatory medications often cannot match — the drug reaches the right location in a concentration that systemic dosing cannot achieve without significant systemic side effects.
Which conditions are most often treated this way
ESI is used for a range of spinal pain conditions characterized by nerve root irritation or compression. The most common include:
- Lumbar disc herniation with radiculopathy — leg pain (sciatica), numbness, or weakness caused by a herniated disc pressing on a lumbar nerve root
- Cervical disc herniation with radiculopathy — arm or shoulder pain, numbness, or tingling from nerve compression in the neck
- Lumbar spinal stenosis — narrowing of the spinal canal that causes leg heaviness, cramping, or pain with walking
- Degenerative disc disease with radicular symptoms — disc breakdown that has caused nerve root irritation
- Post-surgical spine pain — persistent radicular symptoms following disc surgery where inflammation remains a contributing factor
Your physician will review imaging (typically MRI) alongside your symptoms to determine whether the pattern of your pain corresponds to a site where ESI is likely to be effective.
What happens on the day of the procedure
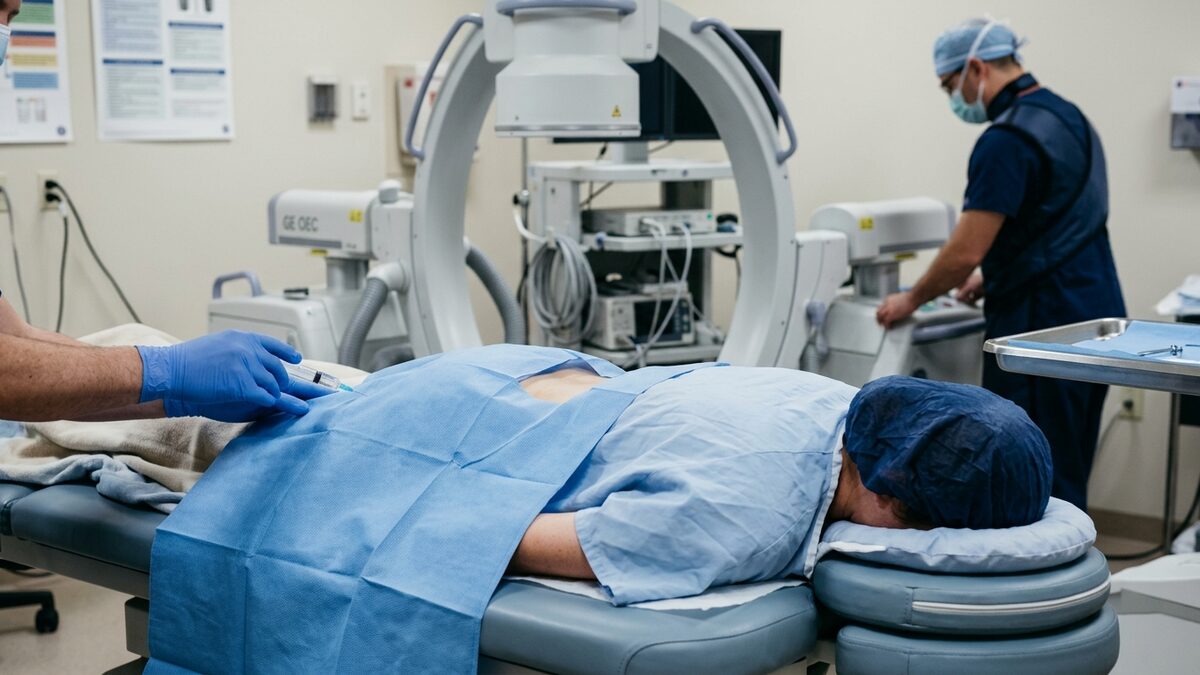
Epidural steroid injections at Axis Pain Group are performed in a procedure room equipped with fluoroscopic (live X-ray) guidance. The use of imaging guidance is standard at our facility — it allows the physician to confirm needle placement before any medication is delivered.
On the day of your injection:
- You will check in and complete a brief pre-procedure review with our clinical team
- An IV line may be placed if sedation is part of your plan; many patients receive only local anesthetic at the skin and proceed without sedation
- You will be positioned face down on the procedure table, and the target area will be cleaned and draped
- Local anesthetic numbs the skin and deeper tissue before the procedural needle is advanced under fluoroscopic visualization
- Contrast dye is typically injected first to confirm epidural spread before the steroid and local anesthetic mixture is delivered
- The injection itself takes a few minutes; the full procedure room time is generally 15 to 30 minutes
Patients who receive sedation will need a driver; patients who receive only local anesthetic may be able to drive themselves, but this should be confirmed with your care team before the appointment.
What to expect in recovery and the days after
Immediately after the procedure, you may notice temporary numbness or a heavy feeling in the injected area or the corresponding limb from the local anesthetic component. This typically resolves within a few hours.
Some patients experience a brief flare of their baseline pain in the first 24 to 48 hours before the steroid takes effect. This is not a sign that the injection has failed. The corticosteroid component typically begins working over 3 to 7 days, with many patients reporting the most noticeable improvement in the first two weeks.
Most patients return to light daily activity the same day. Heavy lifting, strenuous exercise, and activities involving twisting or impact are typically limited for the first 24 to 48 hours. Your physician will give you specific post-procedure instructions.
How many injections are appropriate, and how often
There is no universal answer — the appropriate number of injections depends on your response to the first procedure, the underlying diagnosis, and your overall treatment plan. Most pain physicians limit the number of steroid injections at any given spinal level to three or fewer per year, based on both clinical practice guidelines and considerations around cumulative steroid exposure.
If a first injection produces substantial relief that lasts several months, a second injection when symptoms return is a reasonable discussion. If a first injection produces no benefit at all, the case for a second injection at the same site is weaker, and your physician may recommend reassessment of the diagnosis or a different treatment approach.
When ESI is not the right next step
Epidural steroid injections are not appropriate for all patients with spinal pain. Conditions where ESI is generally not recommended or requires careful evaluation include active infection, certain bleeding disorders or anticoagulant use, uncontrolled diabetes (steroids temporarily raise blood glucose), known allergy to contrast dye or corticosteroids, and pregnancy.
Patients with significant neurological deficits — weakness, loss of bowel or bladder function — typically require urgent evaluation and may need surgical consultation rather than injection therapy.
